What is Chondromalacia Patella?
Tibial Tubercle Osteotomy – Fulkerson Procedure
3D Surgical Animation
The knee is the largest and one of the most complex joints in the human body. The boney structures of the knee consist of the patella (knee cap), Femur (thigh bone), Tibia and Fibula (lower leg bones). The patella glides with knee flexion and extension within the trochlear groove. Gliding of this area is accomplished through articular cartilage under the patella. Articular cartilage is the protective covering over the ends of the bones. Degeneration of this cartilage is called chondromalacia. This allows the joint to glide permitting fluid motion during active and passive activities.
Chondromalacia patella symptoms can be the results of chronic repetitive trauma or the results of an acute trauma in young adults/children. Terms such as movie goer’s knee are commonly used.
Signs and Symptoms
Signs and Symptoms are located within the front or anterior aspect of the knee commonly associated with a dull ache overlying the patella (knee cap). Grinding or crunching can be felt. Pain typically begins gradually and as activity continues symptoms worsen. As they worsen the dull ache can become sharp. Squatting, lunging, running and jumping cause repetitive stress to this area creating unwanted inflammation and pain. The inflammation is due to the softening of the articular cartilage beneath the patella and within the groove of the trochlea.
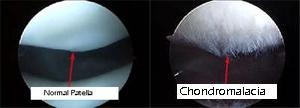
Diagnosis
Diagnosis will be determined through a thorough history and physical examination by a trained sports medicine and orthopedic knee specialist. Examination will consist of palpating the knee complex for pain and a visual examination for deformities. The clinician will check both active and passive range of motion. Specific manual tests will be performed by the specialist to determine if inflammation exists, the amount of weakness, instability and other possible factors causing symptoms. Once the initial diagnosis has been made, radiological examinations may need to take place for further assessment.
Treatment
Treatment for chondromalacia patella is typically non-operatively unless proven otherwise. Non-surgical management includes rest, ice, compression, anti-inflammatory medications, decrease or change of activity levels such as cross training, weight loss, and physical therapy. Surgical management through arthroscopy occurs when a small camera is placed into the knee joint to visualize the damage. During this visualization, ligaments, articular cartilage, meniscus and other soft tissue structures are evaluated. Once the assessment has been completed the surgeon uses a variety of instrumentation to repair, or debride (clean) the knee complex.
Rehabilitation
Rehabilitation is recommended for both surgical and non-surgical management. Regardless of your treatment choice, your sports medicine physician will determine a personalized treatment program that fits your needs. Following the initial onset of signs and symptoms, the initial goal is to reduce pain, increase mobility and range of motion. At home and physical therapy, the use of ice, modalities and specific range of motion and strengthening exercises will be performed several times throughout the day. Pain and anti-inflammatory medication may also be prescribed for additional benefit. The total recovery varies for the condition and the patient. Typically, many will see improvement in symptoms within the first 2 to 4 weeks following the beginning of treatments.
