What is Osteochondritis Dissecans or OCD lesions?
Articular Cartilage Repair
3D Surgical Animation
Microfracture
3D Surgical Animation
The knee is the largest and one of the most complex joints in the human body. It consists of 4 bones, multiple ligaments, muscles and tendons, cartilage and soft tissue. The boney structures of the knee consist of the patella (knee cap), Femur (thigh bone), Tibia and Fibula (lower leg bones). The smoothness motion of the knee is accomplished through articular cartilage and fibrocartilage. Articular cartilage is the protective covering over the ends of the bones. Meniscus or fibrocartilage is the additional type. The purpose of your two meniscuses (medial – inside and lateral – outside) is to act as cushions between your femur (thigh bone) and tibia (lower leg bone). Both kinds of cartilage allow the joint to glide permitting fluid motion during active and passive activities.
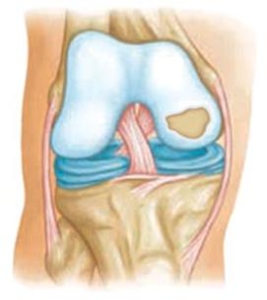
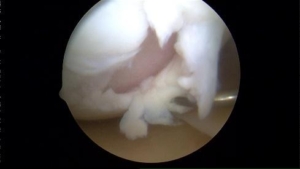
Osteochondritis Dissecans
Osteochondritis Dissecans or OCD lesion is a condition that can occur and develop in children, adolescents and young adults from a decreased blood supply to a specific area of bone affecting the cartilage site. The lack of blood supply causes the cartilage to become damaged and crack and loosen. This does occur in other joints of the body but is more common in the knee. Non-surgical treatment typically consists of partial to non-weight bearing for a period of time, physical therapy, rest and anti-inflammatory conditions. In cases of traumatic injury or in older patients these defects can be surgically repaired or replaced through procedures in which cartilage is transplanted from a cadaver or your own cartilage is grown in a lab and placed back into the area of defect. Above is a photo of a typical OCD lesion within the knee.
Signs and Symptoms
Signs and Symptoms can be located throughout the knee depending on the area of defect. Many will complain of deep knee pain or pain in the back of the joint. Feelings of instability, actual bouts of instability or locking can occur. Pain and swelling are increased with activities such as squatting, lunging, running, jumping if they can be performed. In children and adolescents, a huge effusion (joint swelling) will be present. Grinding and crunching can sometimes be felt within the joint with active and passive movement.
Diagnosis
Diagnosis will be determined through a thorough history and physical examination by a trained sports medicine and orthopedic knee specialist. Examination will consist of palpating the knee complex for pain and a visual examination for deformities. The clinician will check both active and passive range of motion. Specific manual tests will be performed by the specialist to determine if inflammation or joint effusion exists, the amount of weakness, instability and other possible factors causing symptoms. Once the initial diagnosis has been made, radiological examinations may need to take place for further assessment. An MRI (3 dimensional picture) may be ordered to assist in determining the injury. X-rays of the knee complex may be ordered to determine if any bony conditions exist such as fracture or loose bodies or misalignments are present prior to the MRI.
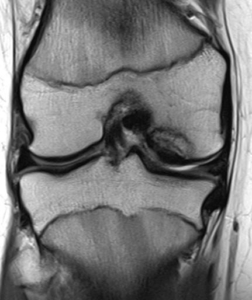
MRI Photo of OCD Lesion
Non-Surgical Treatment or Conservative Management
Non-surgical treatment or conservative management is dependent on the type and area of lesion and involvement. In children and young adolescents, if the lesion is non-displaced, in many cases it can be treated conservatively. As soon as symptoms of pain and swelling resolve they can return to sport or activity without restrictions. In many patients that seek conservative management, it will consist of rest, change in activities, anti-inflammatory (NSAID) medications, Ice 20-30 minutes at times, physical therapy/home exercise program. However, in lesions that are weight bearing affected, displaced, larger than 1cm or those that continue to remain symptomatic then surgical intervention is recommended.
Surgical Management
Surgical management can include either knee arthroscopy to either repair or remove or open procedures to realign or replace the lesion with new cartilage. Both procedures are outpatient.
- Knee arthroscopy, chondroplasty, Drilling, internal fixation, microfracture, loose body removal and diagnostic evaluation, occurs when a small camera is placed into the knee joint to visualize the damage. During the diagnostic visualization, ligaments, bones, and muscles of the knee complex are further assessed by the orthopedic surgeon to determine if you’re a candidate for any additional procedures such as a cartilage transplant procedure. Once the assessment has been completed the surgeon uses a variety of instruments to perform additional tasks that he/she may visualize within the knee:
- Drilling – with a non-displaced lesion – the physician may drill holes into the softened cartilage to stimulate blood flow and the healing of the fragment.
- Internal fixation compression screws are placed into the fragment to hold it in place to allow for healing of the fragment.
- Fragment debridement (removal of loose fragment) or chondroplasty (reshaping of articular cartilage) is performed if the fragment is found to have no bone attached or if it’s unrepairable. Recovery is less than the previous options but may require a second procedure for a cartilage transplant.
- Microfracture – in cases that the fragment cannot be repaired and is removed the defect of bone where articular cartilage has broken away is picked to build a fibrinous cartilage cap. A period of non-weight bearing activity may be prescribed. Total recovery is 3-4 months.
- Open cartilage Transplant options. These procedures are also outpatient. Physical therapy is required and each type of transplant has specific protocols pertaining to the healing and benefit of the patient. Below are some of the options available. If you are a candidate, your physician will recommend and discuss during your consultation.
- MACI® (autologous cultured chondrocytes on porcine collagen membrane) is an autologous cellularized scaffold product that is indicated for the repair of single or multiple symptomatic, full-thickness cartilage defects of the adult knee, with or without bone involvement. MACI is the first FDA-approved product that applies the process of tissue engineering to grow cells on scaffolds using healthy cartilage tissue from the patient’s own knee.
- Allograft OATS or Osteochondral Allograft Transplantation Surgery replaces damaged articular cartilage from a cadaver donor. During the open procedure, your defect is area is first debrided (cleaned). Then an exact measurement is taken of the defect. A core of bone and cartilage is removed from the fresh cadaveric donor. Finally, your new cartilage is press fit into the previous defect site. The below link/video will review how the procedure is performed.
- DeNovo® NT Graft is a particulate juvenile cartilage implant used for the repair of articular cartilage damage. It is intended to provide surgeons with an early-intervention option for articular cartilage repair and cartilage restoration. The juvenile cartilage cells or implanted in a single stage procedure with fibrin fixation.
